Introduction
|
|
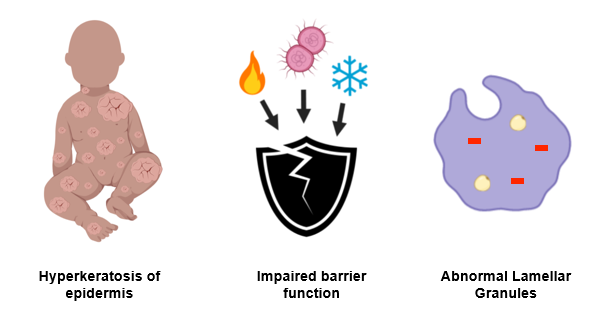
Harlequin ichthyosis is a rare autosomal recessive disease cause by a mutation in the ABCA12 gene. The disease affects the outer layer of skin (the epidermis), causing a f. The disease phenotype is found to be the worst in newborns, with only around fifty percent surviving past the first year of life. Those who survive see a lessening of severity in the disease, but still face health issues and social stigma due to their appearance. HI is characterized by three main symptoms, hyperkeratosis of the epidermis (thickening of the skin), impaired skin barrier function, and abnormal lamellar granules.
|
ABCA12 Gene
|
Mice as model organisms
|
|
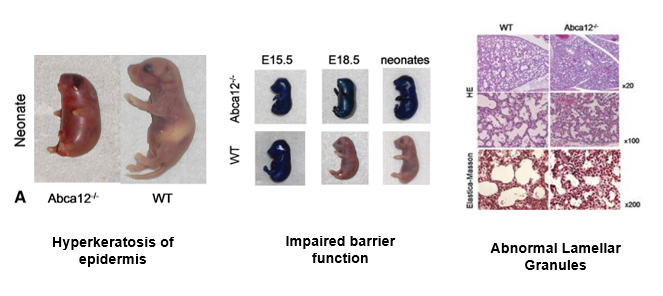
I chose mice as my model organism because they have historic use in HI studies, and the ABCA12 gene and its domains are highly conserved between them and humans. The assays I will be conducting in aims 1-3 have been previously performed by HI researchers, with their models pictured below. The first assay is for hyperkeratosis of the epidermis, which can be visually observed and quantified by measuring thickness of skin punches between wild-type (WT) and ABCA12 mutant mice. The second assay is for impaired barrier function. WT and mutant embryos at different developmental ages are placed in a beaker of toluidine blue dye. When the skin has properly developed, it acts as a a barrier between the organism and the environment, so we can see ABCA12 mutant mice have impaired barrier function because they take up the toluidine dye. The third assay is for examining lamellar granules with strong microscopic magnification. WT lamellar granules are more round in shape, and contain more lipid molecules compared to their ABCA12 mutant counterparts.
|
Gap in knowledge
|
|
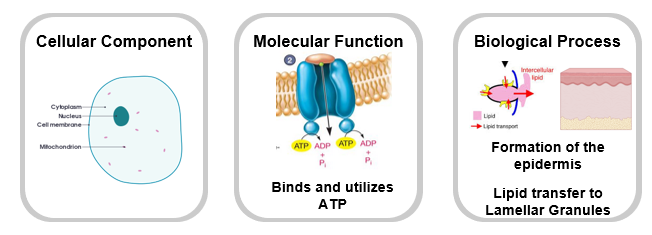
We know ABCA12 mutations cause abnormal lamellar granule formation, and that abnormal lamellar granules result in an increase of hyperkeratinizaiton, and a decrease in lipid transport. However, how ABCA12 mediates this in the epidermis remains unclear.
|
Aim 1: Identify amino acids in ABCA12 necessary for lamellar granule formation in the skin
|
|
My first aim is to identify conserved amino acids in the ABCA12 AAA-transport domain that may be important for lamellar granule formation and lipid transport in the epidermis.
|
Aim 2: Identify differentially expressed genes important for lamellar granule formation in the skin.
|
|
My second aim is to use RNA-sequencing to identify differentially expressed genes important for lamellar granule formation. This gene expression data will be organized by GO terms and quantitative expression level.
|
Aim 3: Identify proteins important for lamellar granule formation in the skin and quantify their expression.
|
|
My third aim is to identify novel protein interactions that may be involved in the formation of lamellar granules and the epidermal layer.
|
Future Directions
|
|
There is no cure for harlequin ichthyosis, and current treatments center around trying lessen symptoms that affect daily life. Topical and oral retinoids are the most common treatment for HI, as they encourage proper skin formation, decreasing hyperkeratinization. Some gene therapies are currently being tested, and I would be interested in examining ones that focus on restoring lamellar granule formation to WT levels, as lamellar granules are the driving force of keratin shedding.
|
| final_hi_presentation.pptx |
| Seablom.2.21.20.ppt |
This web page was produced as an assignment for Genetics 564, an undergraduate capstone course at UW-Madison